Infant mortality rates serve as a critical indicator of public health and welfare, reflecting deeper issues within healthcare systems. Alarmingly, recent studies have shown that these rates for Black infants have not only remained disproportionately high but have worsened compared to their white counterparts. While overall mortality rates between Black and white Americans have improved, the stark reality is that Black infants die at twice the rate of white infants. This disparity highlights significant racial inequalities in health, underscoring systemic challenges that continue to plague the healthcare system. Addressing these racial disparities in health outcomes is vital for shaping effective public health policy that can genuinely improve life expectancy for all Americans, particularly marginalized communities.
When discussing the tragic phenomenon of infant deaths, we often touch on critical health statistics that reveal an unsettling reality. The persistent and growing divide in mortality rates among newborns of different racial backgrounds, particularly the struggles faced by African American infants, underscores a significant public health challenge. The systemic issues rooted in healthcare inequality are contributing factors that must be examined to improve life outcomes for this vulnerable population. Efforts to bridge these gaps must prioritize understanding the underlying causes of increased mortality and reshape public health strategies accordingly. Addressing these issues with a holistic and informed approach could lead to equitable healthcare access and significantly reduce these alarming mortality rates.
Understanding the Widening Gap in Infant Mortality Rates
The alarming increase in infant mortality rates between Black and white Americans poses a pressing public health issue. Research shows that while the overall mortality rates have improved significantly for both racial groups, the disparity in infant mortality has widened alarmingly. As of today, Black infants die at a rate that is double that of white infants. This stark reality highlights a systemic inequality that has persisted over decades, indicating that improvements in healthcare access and quality have not been equitably distributed across racial lines.
Several factors contribute to the ongoing disparities. Medical conditions during pregnancy have emerged as leading causes of excess deaths among Black infants. This underlines the complex interplay of healthcare accessibility, socioeconomic status, and systemic racism that influences health outcomes. Understanding these underlying reasons is crucial for creating effective public health policies targeted at reducing these disparities, ensuring that the health of infants is recognized as a priority regardless of race.
The Impact of Racial Disparities on Health Outcomes
Racial disparities in health outcomes extend beyond mere statistics; they reflect a reality where marginalized communities face significant barriers to maintaining health and well-being. The data revealing a widening gap in infant mortality rates illustrates a troubling trend that calls for urgent intervention. Black Americans, despite improvements in overall life expectancy, still grapple with a healthcare system that inadequately addresses their unique needs, often resulting in poorer health outcomes.
In addition to lack of access to quality prenatal care, factors such as socioeconomic status and environmental influences further contribute to these disparities. Public health policies must be aware of these intricacies to effectively mitigate racial health disparities, particularly in vulnerable populations. It is critical for stakeholders to act decisively to dismantle these barriers and ensure equitable access to health resources for all racial groups.
Healthcare Inequality and Its Consequences
Healthcare inequality is a multifaceted problem that has dire consequences for communities, particularly among Black Americans. The consistent rise in infant mortality rates underscores the need to address not only access to care but also the quality of that care. The situation is aggravated by systemic racism, which often leads to disparities in treatment options and health education. Reducing healthcare inequality should be a central focus of public health initiatives to foster an environment where every individual, regardless of race, can access the care they require.
Moreover, addressing healthcare inequality involves ensuring that medical practitioners are culturally competent and sensitive to the unique needs of diverse populations. Training and reform at the institutional level are necessary to create a healthcare system that prioritizes equity and inclusiveness. Emphasizing community-based interventions that consider the social determinants of health will play a critical role in bridging these gaps and ultimately improving health outcomes for Black infants and their families.
Public Health Policy: The Path Forward
The findings of the recent study illuminate the critical need for effective public health policies that specifically target the disparities in infant mortality rates. Policymakers must prioritize the allocation of resources to communities with the highest rates of infant mortality, focusing on equitable healthcare strategies. By implementing comprehensive public health initiatives that address both access and quality of care, it is possible to make significant strides in improving health outcomes for Black infants.
Future public health policies must adopt a holistic approach that integrates education, healthcare access, and community support systems. Strategies could include increasing funding for prenatal and postnatal care services in underrepresented areas, enhancing maternal health education, and fostering partnerships with community organizations. By creating a framework that actively combats racial disparities in health, public health authorities can ensure that the health and lives of infants are prioritized — ultimately leading to reduced infant mortality rates across racial groups.
Life Expectancy and Racial Discrepancies
Despite notable improvements in life expectancy for both Black and white Americans over the past several decades, the disparities present underscore an ongoing issue within the healthcare system. Data shows that while Black Americans have seen an increase in life expectancy, this has not translated into improved health outcomes for the Black infant population. The troubling fact that Black infants are dying at a rate significantly higher than that of their white counterparts raises questions about the effectiveness of measures taken to address racial health disparities.
Understanding the nuances of these statistics is vital for addressing the root causes of racial discrepancies in life expectancy. A multifactorial approach is essential, examining elements such as socio-economic status, access to quality education, and systemic inequities within the healthcare system. With a concerted effort to explore and understand these issues, public health initiatives can better target interventions that address the underlying factors affecting the health and wellbeing of Black infants specifically.
Exploring the Causes of Excess Deaths Among Black Infants
Identifying the causes of excess infant mortality among Black Americans is a critical step toward reducing these tragic outcomes. Medical factors, including complications during pregnancy and inadequate prenatal care, have been highlighted as leading contributors to the higher mortality rates. However, this issue cannot be analyzed in isolation; social determinants of health also play a significant role. Factors such as poverty, education level, and neighborhood safety must be considered when exploring this health crisis.
Research indicates that the quality of medical care for Black mothers often differs from that received by their white counterparts, which contributes to a higher incidence of complications and mortality rates among their infants. By emphasizing targeted research into the multifaceted causes of these disparities, public health officials can devise interventions that address both medical and social issues affecting Black infant mortality. Collaborative efforts across disciplines will be crucial in implementing sustainable change that protects vulnerable populations.
The Role of Community in Public Health Initiatives
Community engagement plays a vital role in addressing health disparities, particularly in preventing infant mortality. Local organizations and leaders are often best positioned to understand the unique challenges faced by their communities, making their involvement essential for developing effective public health strategies. Collaboration with community members can help identify specific needs and tailor interventions to be culturally effective and relevant.
Programs that empower communities through education and resources can lead to better health outcomes. Initiatives could focus on improving access to prenatal care, providing parenting classes, and creating supportive networks for expecting and new mothers. By harnessing the power of community-driven initiatives, public health officials can foster environments conducive to healthier lifestyles, ultimately reducing the risk of infant mortality rates among Black Americans.
The Importance of Racial Equity in Healthcare
Achieving racial equity in healthcare is paramount to addressing the systematic issues that contribute to disparities in health outcomes. As the data suggests, healthcare inequality remains a pressing challenge that disproportionately affects Black infants. Addressing these disparities requires a commitment to dismantling systemic barriers that prevent equitable access to quality care.
Public health policies must be designed with an equity lens, ensuring they are inclusive and address the specific needs of diverse populations. This might include increased funding for healthcare facilities in underserved areas, investment in training for healthcare providers on cultural competency, and efforts to include voices from marginalized communities in policy development. By prioritizing racial equity, the healthcare system can work towards a future where every infant, regardless of their race, has an equal chance at a healthy start in life.
Future Directions for Research in Infant Health Disparities
The ongoing disparities in infant mortality rates necessitate further research into the underlying causes. Comprehensive studies that explore the multifactorial aspects of health disparities are essential to inform public health policy. By analyzing data that spans several decades, researchers can identify trends and potential interventions that could significantly impact the health of Black infants.
Future research should focus on both quantitative and qualitative data, investigating not only the statistical realities of health disparities but also the lived experiences of individuals affected by them. Engaging with communities directly will provide valuable insight into the factors contributing to infant mortality and inform actionable strategies that can be implemented at the policy level. By prioritizing research and data-driven approaches, public health officials can make informed decisions that may ultimately save lives.
Frequently Asked Questions
What are the current trends in infant mortality rates among Black infants in the U.S.?
Current trends indicate that Black infants in the U.S. have a significantly higher mortality rate compared to white infants. Specifically, Black infants die at twice the rate of their white counterparts, a troubling statistic that highlights ongoing racial disparities in health.
How do racial disparities in health affect infant mortality rates?
Racial disparities in health have a profound impact on infant mortality rates. For Black infants, systemic healthcare inequalities contribute to higher mortality rates, underscoring the necessity for targeted public health policies to address these gaps.
What factors contribute to the healthcare inequality affecting Black infant mortality rates?
Healthcare inequality affecting Black infant mortality rates stems from several factors, including limited access to quality prenatal care, socioeconomic disparities, and systemic racism within healthcare systems, all of which contribute to a higher risk of medical complications during pregnancy.
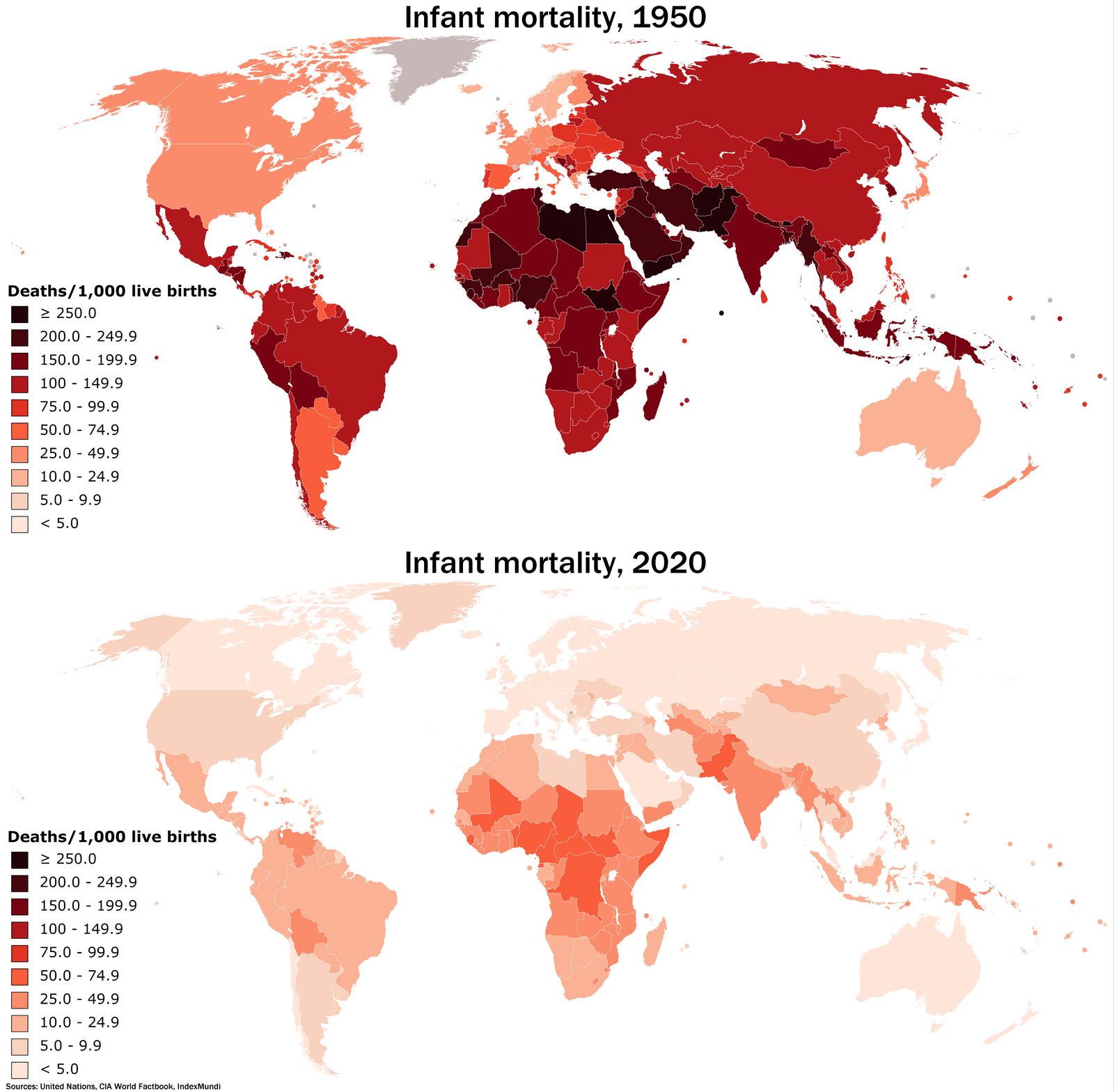
Why has the gap in infant mortality rates between Black and white infants widened since the 1950s?
The gap in infant mortality rates between Black and white infants has widened since the 1950s due to persistent healthcare inequalities and insufficient public health interventions aimed specifically at addressing the unique needs of Black mothers and infants.
What steps can public health policy take to address disparities in infant mortality rates?
Public health policy can address disparities in infant mortality rates by implementing comprehensive prenatal care programs, increasing funding for maternal health services in underserved communities, and promoting education on maternal health among Black mothers to reduce risks associated with infant mortality.
How does life expectancy for Black Americans relate to infant mortality rates?
While life expectancy for Black Americans has increased significantly over the decades, the infant mortality rate remains disproportionately high compared to white Americans, indicating that improvements in life expectancy do not necessarily equate to equal healthcare outcomes for infants.
What can be done to improve healthcare access for Black mothers to reduce infant mortality?
Improving healthcare access for Black mothers involves increasing the availability of quality prenatal and postpartum care, offering education and support programs tailored to their needs, and addressing the broader societal factors that contribute to healthcare disparities.
What impact does community support have on addressing Black infant mortality rates?
Community support plays a critical role in addressing Black infant mortality rates by fostering environments that promote health education, access to healthcare resources, and emotional support networks, which are essential for improving maternal and infant health outcomes.
| Key Points | Details |
|---|---|
| Overall Mortality Rates | Mortality rates between Black and white Americans have narrowed since the 1950s, highlighting an overall increase in life expectancy for both groups. |
| Infant Mortality Rates | Black infants die at twice the rate of white infants, with a 115% increase in the disparity since the 1950s. |
| Life Expectancy | Life expectancy for Black Americans rose from 60.5 years to 76 years; for white Americans, it increased from 69 years to 79.3 years. |
| Causes of Infant Death | Medical conditions during pregnancy have been identified as leading causes of the excess deaths among Black infants. |
| Call to Action | The study emphasizes the need for public policy to address healthcare disparities that contribute to unequal infant mortality rates. |
Summary
Infant mortality rates are a significant public health concern, particularly the alarming disparity observed between Black and white infants. Despite advancements in healthcare and improved life expectancy for adults, Black infants continue to experience significantly higher mortality rates compared to their white counterparts. This highlights a critical area for policy intervention and healthcare reform, aiming to ultimately equalize health outcomes and reduce unnecessary infant deaths in the future.